As a result of the COVID-19 pandemic, it is a challenge for the scientific community to publish results quickly, and publication often occurs at the price of quality and reproducibility, which in turn undermines the public’s trust of science. A recent paper by Gaiha et al evaluated the relation between youth smoking and coronavirus and concluded, “COVID-19 is associated with youth use of e-cigarettes only and dual use of e-cigarettes and cigarettes.” If this is true, this finding has major implications for policy and would justify strong additional calls for youth not to use these products during the pandemic. However, we question the accuracy and credibility of this study’s conclusions. A similar case occurred last year concerning a study that cited a link between heart attacks and vaping, by Stanton Glantz; the study was recently retracted because of unreliable results.
In the Gaiha study, smoking or vaping status was defined as use of tobacco products ever or during the past 30 days. COVID-19 information was collected by asking participants whether they had been tested and whether they were diagnosed as positive. Both smoking/vaping status and COVID-19 status were based on a self-report survey, without verification. The authors calculated odds ratios to estimate the association between using tobacco and testing positive for COVID-19 among 2,183 e-cigarette users and 2,168 never-users. Rather than including only respondents who were tested for COVID-19, they considered the entire survey population to evaluate risk. However, the e-cigarette users were approximately 3 times more likely to get tested than were never-users, which leads to a greater number of COVID-19–positive diagnoses. In fact, the likelihood of users and non-users testing positive for COVID-19 is similar if one compares only those who were tested in each group.
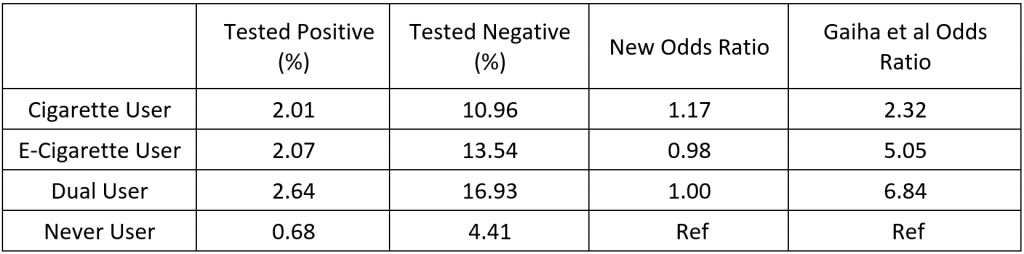
The odds ratio helps us understand the measure of association between two events, or the risk of an event in an exposed group versus an unexposed group. We recalculated the odds ratios using the supplementary data cited in the article, assuming all COVID-19–positive diagnoses were tested, and we replaced the control group with negative test cases (total tested in each category minus the total who tested positive). This calculation produced much smaller odds ratios for the risk of COVID-19–positive diagnoses for inhaled tobacco product users versus never-users.
Table 1: Odds ratios for association between COVID-19–positive diagnosis and use of inhaled tobacco products in ever-users
There are other factors that the authors overlooked when reaching their conclusions. Since the study was based on self-report, fixed-choice questions and reporting bias may have lowered the validity and reliability of the data. The survey defined COVID-19 symptoms as cough, fever, tiredness, and difficulty breathing. Therefore, it is possible that respondents confused symptoms of the common cold and flu with the symptoms of COVID-19 infection, which might exaggerate the number of participants who reported COVID-19–related symptoms. Baseline data showed that e-cigarette users were less likely to be complying with shelter-in-place orders, and people who are vaping are of course not wearing masks while doing so. A lack of specific geographic or occupational information for the participants reduces the ability to focus on high-risk populations, although the authors found an odds ratio of 5 for a COVID-19–positive diagnosis among participants from states having 11% to 20% COVID-19–positive cases. It is possible that participants were infected by family members or others, which would blur the role of tobacco use. Further, the paper does not take into account the temporal association between testing and product use, as the odds ratio (OR; 95% CI) for ever-users (5.05 [1.82-13.96]) was higher than that for current users (past 30 days; 1.91 [0.77-4.73]). The authors claim that using tobacco products is a “significant risk factor,” yet finding an association between vaping and a COVID-19 diagnosis does not prove causation.
Research papers should go through a stringent vetting process before being published, and this is especially true during a public health emergency when study findings are likely to gain immediate public attention and policy response. Even under the best of circumstances, published research findings are quite likely to be false for several reasons, including faulty methodology. Our analysis demonstrates that a modified application of the data using a similar methodology generates a much different outlook than currently presented. The Foundation strongly encourages evidence-based science that uses proper methodology and sound reasoning.
© 2023 Foundation for a Smoke-Free World. All rights reserved.